By Cayden Antee, Synergy Strive TMS Treater (Silver Spring, MD)
In recent years, transcranial magnetic stimulation (TMS) therapy has grown rapidly in the treatment of major depressive disorder. Less discussed, however, is the utility of TMS therapy in the treatment of obsessive-compulsive disorder (OCD).
While many questions arise regarding effectiveness, insurance coverage, and safety, many who are considering TMS for OCD would like to know how it helps. Because the neuroscience of OCD and TMS are each incredibly complicated (and ever-changing), we’ll provide an accessible description of what’s biologically happening when undergoing TMS therapy for OCD.
One of the most essential functions of every brain—from those within houseflies to those within humans—is the ability to identify and subsequently avoid sources of danger. Here, it’s clear that all brains would be well-advised to err on the side of caution, as it’s adaptive to be excessively cautious as opposed to needlessly risky. Another adaptive function of the brain is the ability to carry on after verifying that danger is, indeed, absent.
Though I’m at risk of oversimplifying a very complex (and heterogeneous) condition, OCD may be best conceptualized as a disorder in the brain’s ability to accurately detect, evaluate, and move on from these threats. OCD is sometimes characterized as a “stuck gas, broken brake” in the threat-detection and threat-avoidance system. While non-OCD brains can accurately detect and appropriately avoid danger, those with OCD overestimate threats (stuck gas) and struggle to accept the lack thereof (broken brake).
While mental processes don’t perfectly map onto brain regions, it’s safe to purport that the neurological network most associated with this system is the cortico-striatal-thalamo-cortical (CSTC) pathway—what a mouthful! Put simply, OCD is strongly associated with the hyperactivity of this network, potentially the cause of heightened threat sensitivity, compulsivity, and habit formation.
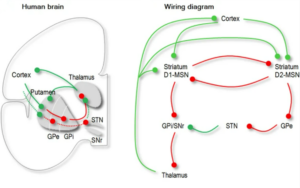
Conceptual visualization of the CSTC system (Rădulescu et al., 2017)
The central feature of TMS therapy is its ability to strengthen brain regions and their related pathways. To do so, a magnetic coil (rested on a patient’s head) repetitively stimulates brain cells, causing them to reinforce their connections with each other, thereby increasing their capacity to serve their respective functions.
Given this ability, TMS can fit perfectly within OCD, as it strengthens the brake of the aforementioned “stuck gas, broken brake” pathway. Here, the “brake” is the medial prefrontal cortex, a subregion associated with (among other things) the cognitive regulation of threat detection. Although TMS cannot treat the entire CSTC network, we can strengthen the component that is best-poised to regulate it.
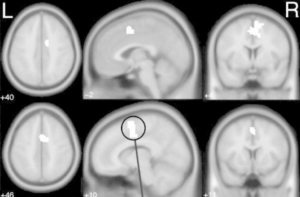
Medial prefrontal cortex activation in OCD-diagnosed patients (Kaufmann et al., 2013)
By strengthening this area of the frontal cortex, we’ve seen (both in the research and in our clinical practice) remarkable improvements in OCD symptoms like checking behaviors, rituals, and more (all of which are downstream of atypical threat detection).
If you’d like to learn more about TMS for OCD, or are interested in beginning TMS therapy, we’d love to help. You can fill out the contact portal on this page or give us a call! We offer insurance-covered TMS therapy for depression and OCD in Columbia, Towson, and Silver Spring, MD.